Happy New Year! And welcome back to FED! I have a lot planned for 2026, but before we get into any of it, I want to start by unpacking something unexpectedly buzzy: the Dietary Guidelines for Americans (DGAs).
I’ve been a dietitian for decades, and I’ve never seen this much attention given to the release of the DGAs. If you’re unfamiliar with the DGAs, you’re not alone. Historically, they’ve been read by dietitians, nutrition researchers, and public health officials. That was the audience. Apparently, it isn’t anymore.
So I’m using the first post of 2026 to explain what they are, what they actually say, and how an average person should think about it - without politics or pearl-clutching.
There’s been plenty of political framing around this release—favorable takes from those aligned with the current administration, sharper scrutiny from those who aren’t. I’m going to leave the policy and politics to people who specialize in that. What follows is a practical look at what the guidelines say and how to use them when thinking about the food you and your family actually eat.
The timing was interesting. I was in Japan when the guidelines were released. Japan is often held up as the poster child for a “healthy traditional diet”—fresh fish, vegetables, rice, simple preparations. And yes, that foundation is still very much there. But Japan is also not immune to the global creep of fast food and ultra-processed meats. Case in point: this ad for a Burger King burger made with a full pound of beef (!)
It’s a useful reminder that questions about what we eat—and how modern food environments shape those choices—aren’t uniquely American problems. Healthy dietary patterns are a global need, not a niche wellness concern.
Let’s start with the basics: What are the Dietary Guidelines for Americans?
The Dietary Guidelines for Americans (DGAs) are the federal government’s recommendations for how Americans should eat to support health and reduce the risk of chronic disease.
Updated every five years, the guidelines are meant to provide a population-level framework for healthy eating over time. It’s not a personalized diet plan or instructions for what to make for dinner tonight.
Importantly, the DGAs directly influence:
School lunch and breakfast programs
WIC and other federal nutrition assistance programs
Public health messaging and education
How clinicians and dietitians are trained to think about dietary patterns
In other words, even if you’ve never read the DGAs, you’ve almost certainly felt their impact.
So, what are the new Guidelines recommending?
At a high level, the message is familiar, and to their credit, delivered directly.
The guidelines emphasize building meals around “real food.” The term isn’t explicitly defined and appears intentionally open to interpretation, but it generally refers to whole and minimally processed foods such as vegetables, fruits, beans and lentils, nuts, seafood, lean meats, eggs, and dairy.
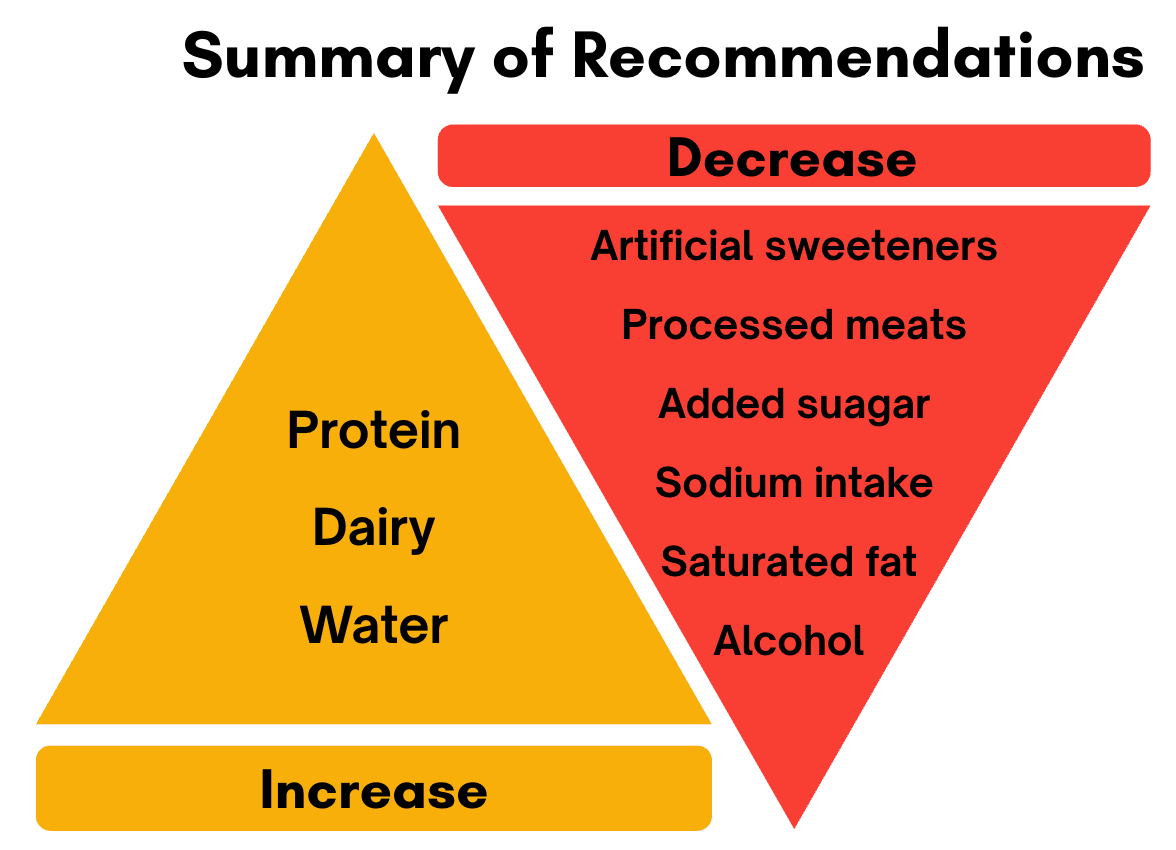
A few key recommendations stand out:
And if you are looking for more specifics:
Sounds like solid advice.
Some of it, yes. Here’s what I like about them:
They are simple and readable
The document is short, written in plain language, and easy to follow. That matters. Nutrition guidance is often buried in jargon or framed in ways that make it inaccessible to the very people it’s meant to serve. If the goal is broad understanding, clarity is doing real work here.
The focus is on food, not nutrients
The emphasis on “real food”, even without a strict definition, moves the conversation away from nutrient math and toward dietary patterns. That’s a meaningful shift. People eat meals, not spreadsheets.
Clear limits on processed meats
The recommendation to avoid or significantly limit processed meats is stated more directly than in previous versions and aligns with long-standing evidence. (Refer to my prior post on processed meats.)
Guidance on sugars, sweeteners, and sodium
Limiting added sugars and artificial sweeteners, and reducing sodium from packaged foods aren’t new ideas, but the straightforward framing is solid.
Mentions the role of fiber and fermented foods in gut health.
Fiber and fermented foods are noted for their role in gut health, though only in passing. It’s a welcome inclusion, though one that could have been emphasized more. (Refer to my prior posts on fiber and fermented foods.)
So why the controversy?
Because guidance that looks reasonable on paper can get complicated fast in real life.
The recommendations aren’t extreme, but when you try to apply them, some gaps become hard to ignore.
Portion size
The document advises eating “the appropriate amount of calories for your needs.”
That sounds sensible. It also stops short of being useful.
How someone determines an appropriate amount of calories is left unanswered. Portion size directly affects calorie intake, which influences weight, metabolic health, and chronic disease risk. If individuals are expected to apply this guidance, this is a notable omission.
No guidance on alcohol or fiber intake
Fiber is encouraged, and alcohol is advised to be limited, but specific intake amounts are not provided. Those numbers would be useful for interpretation and application.
Saturated fat
The long-standing recommendation to keep saturated fat below 10% of total calories remains, and it’s supported by evidence.
At the same time, the guidelines encourage foods and fats such as olive oil, butter, full-fat dairy, red meat, and beef tallow.
Here’s where the tension shows up. Olive oil fits easily within that limit. Butter, full-fat dairy, and beef tallow do not, unless used sparingly. But portion guidance isn’t addressed. (Refer to my prior post on full-fat dairy and beef tallow.)
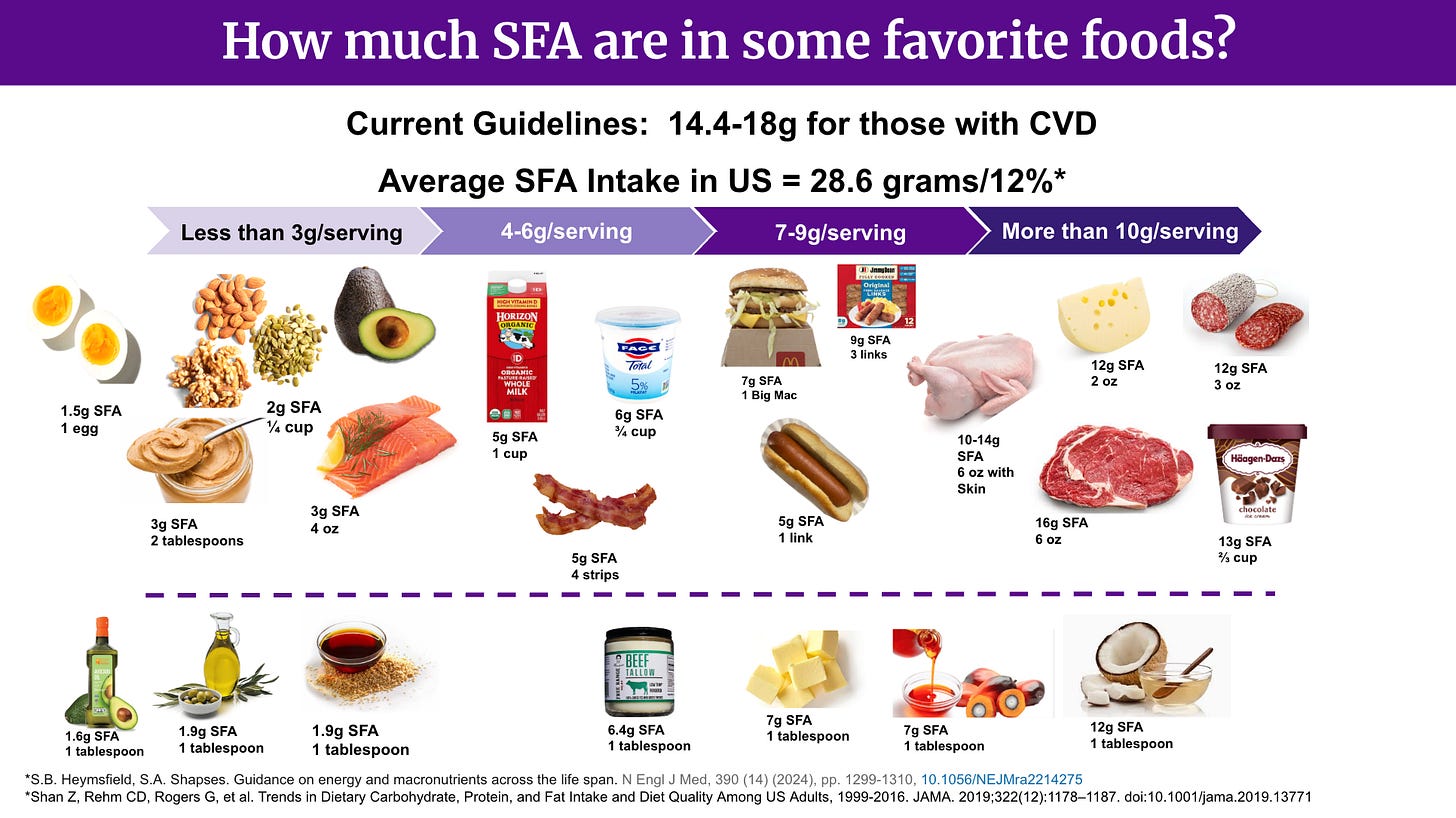
The slide shown below, from a presentation I delivered at the NYU Cardiovascular Lifestyle Medicine Conference, illustrates how Americans already exceed saturated fat recommendations. The cap hasn’t changed, but the food guidance has. The question is unavoidable: how are you supposed to do both?
Protein at every meal
Protein recommendations increased—nearly doubling what older guidance emphasized.
Raising protein intake without also increasing calories or saturated fat requires thoughtful choices. A ribeye and ground beef (found at the top of the inverted pyramid) technically count, but they don’t land the same as salmon, shrimp, beans, or lentils, even when protein numbers look similar on paper. The guidelines don’t clearly address that tradeoff.
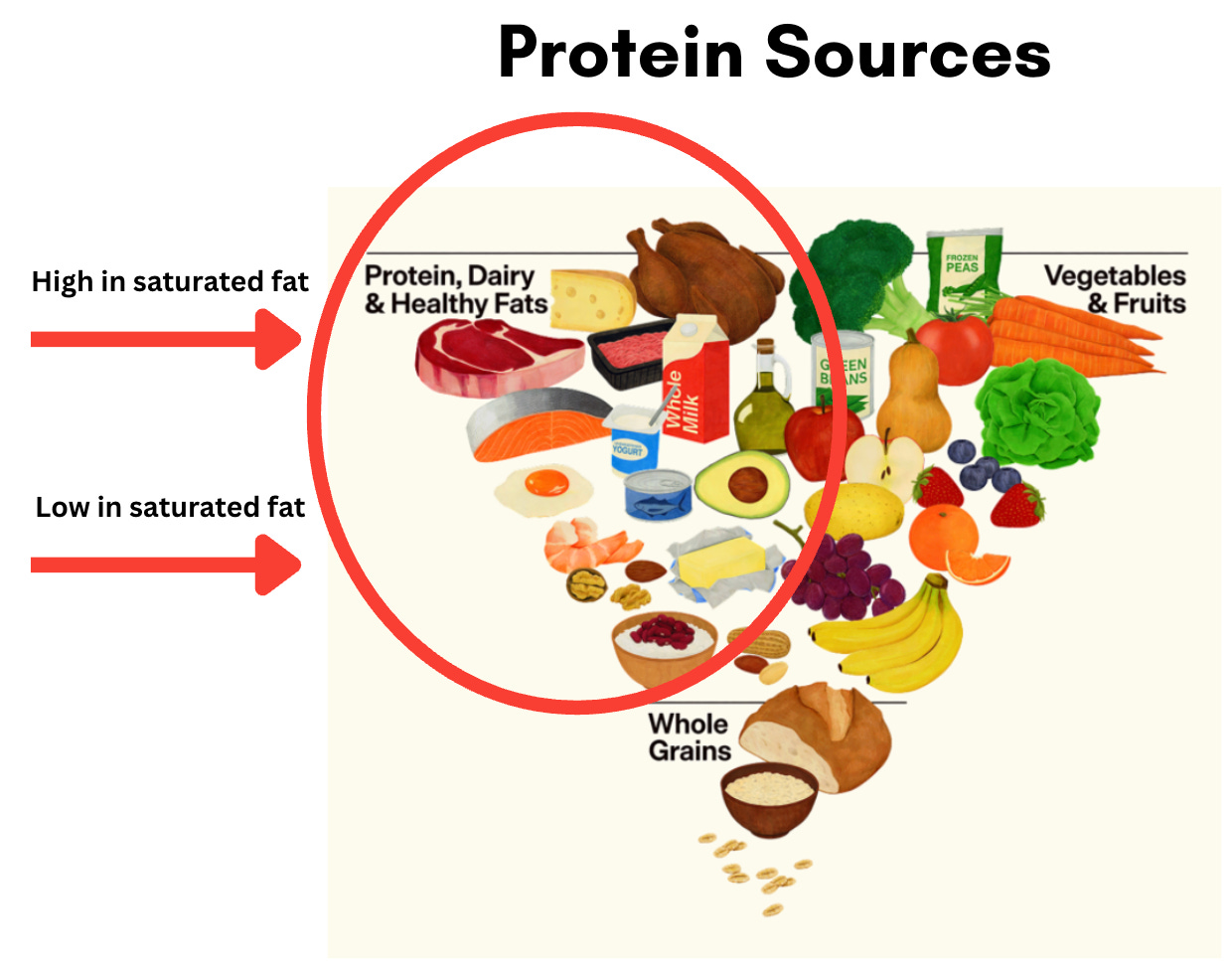
Affordability
The document notes that efforts are underway to make these recommendations affordable. For now, that’s aspirational.
This matters because the DGAs aren’t meant to guide individual diets; they’re meant to inform programs like school meals and WIC. Many of these programs are facing budget constraints and, in some cases, cuts. How higher-cost food recommendations are expected to be executed under tighter budgets is unclear.
Some “real foods,” particularly animal proteins, are expensive. Others like beans, lentils, and frozen vegetables, are among the most affordable foods available. Meanwhile, fast food and packaged meals remain cheap, quick, and accessible. That reality shapes behavior, and the guidelines don’t meaningfully address it.
So, how should I interpret all of this?
It depends on who you are.
If you’re a clinician
Protein needs increased, but source matters. Emphasize fish, shellfish, lean meats, beans, lentils, tofu, and edamame.
Encourage fatty fish like salmon for omega-3s.
Keep saturated fat in view. Butter and fatty meats shouldn’t dominate the plate.
Talk about portions. Start with what someone is actually eating, then adjust.
Don’t forget fiber. There’s no protein deficiency crisis in the U.S., but there is a fiber one, which is linked to gut health, glucose control, and cardiovascular risk.
Discuss dairy thoughtfully. Are there intolerances, allergies, or plant-based preferences? If so, address calcium, vitamin D, and protein elsewhere.
Ask about artificial sweeteners. The evidence isn’t conclusive, but understanding why someone uses them—diabetes management, calorie control—matters for counseling.
Ask about alcohol. Is it social and moderate, or isolated and excessive? Context matters.
If you’re just trying to eat dinner
Here’s the plain-English version:
Build most meals around foods that don’t come from a box or bag.
“Real food” looks like seafood, lean meats, beans, lentils, fruits, vegetables, nuts, eggs, dairy, olive oil, and avocado oil.
Fiber matters. Fiber is a carbohydrate. Remove carbs entirely, and fiber goes with them.
Beans and lentils are fiber powerhouses. Fruits and vegetables help, but legumes do the heavy lifting.
Processed foods happen. This is 2026. When you use them:
Look for short ingredient lists
Aim for ≥5 g fiber per serving when it makes sense
Remember, not all good-for-you foods contain fiber - yogurt, eggs, dark chocolate get a pass.
Look for no added sugar, or keep it under ~5 g per serving—or ~10 g per meal
And yes, you can still eat cookies, ice cream, chips, and treats. Just try not to do it absentmindedly while scrolling your phone. Your brain deserves to be present for dessert.
The science hasn’t dramatically changed, but the conversation has. The Guidelines provide structure, not certainty, and they work best when paired with context, common sense, and realistic food choices.













Just thank you...I needed this article... Cheers from Eugene, OR
This was a clear and concise explanation. Thank you!