Let's Talk About Weight
A conversation with intuitive eating dietitian Nicole Groman on stigma, GLP-1s, and health beyond BMI.
Whenever someone learns I’m a dietitian, the conversation almost always pivots to diets and weight.
Keto. Fasting. “How do I lose 10 pounds?”
I’ve come to accept it as an occupational hazard.
What we eat matters. But it’s dietary patterns over time that shape health, not the fad diet followed for a few months before life (and hunger) returns. And then there’s weight. It’s tied to health, yes, but not always in the ways people assume. We don’t blink at the thin person who lives on takeout and sleeps four hours a night. But a person in a larger body ordering lunch? That plate is judged.
The stigma feels louder than ever.
So I wanted to talk about it with someone who works in this space every day.
Nicole Groman, known online as @thehungryclementine, was once my student. I’ve watched her professional evolution with pride. She now practices in the intuitive eating and body neutrality space — an area often misunderstood, even within dietetics. Even by me.
I had questions. She had answers.
I sat down with her and turned the tables. The student became the teacher. Here’s our conversation, edited and condensed for clarity.
From Gym Culture to Graduate School
Lourdes Castro: Do you remember the first time you realized dietetics was a field you could study and turn into a career?
Nicole Groman: I remember the first time I decided that’s what I wanted to do. I don’t remember the first moment realizing it could be studied as a career. I don’t know if I ever had that thought. The first time I even considered it was when I was changing my major at Cornell. It was going to be either psychology or nutrition. I actually chose psych because I didn’t feel like doing the nutritional biochem.
LC: You can run, but you can’t hide from biochem.
NG: Exactly.
After graduating, Nicole didn’t know exactly what she wanted to do. She started working at a gym. That’s where things shifted.
NG: Through working at the gym, I got introduced to fitness culture - for better or for worse. I started exercising more regularly and getting nutrition advice from people who really shouldn’t have been giving it. Trainers are fitness experts, not nutrition experts. That’s where I learned about the “cheat day.” I became quite obsessed with nutrition.
Then I had a lightbulb moment. I was standing in my parents’ kitchen, in front of the stove, and it hit me: I can combine talking about food and nutrition with building client relationships and become a nutritionist. That was the word I used, because I didn’t even know dietitians were a thing. That’s what led me to apply to NYU for my master’s in nutrition.
But the obsession wasn’t healthy.
NG: Halfway through graduate school, I started working with a therapist and then a dietitian because I realized I had my own stuff to deal with. When I finished working with my dietitian, I naturally entered into intuitive eating, the food freedom space, because of my own experience.
When “Healthy” Isn’t Healthy
NG: I didn’t know I was struggling with my relationship with food. I knew something felt off, but I didn’t realize I was in an unhealthy obsession with healthy eating. I thought I was doing everything right, avoiding sugar during the week and only eating it once. It was orthorexia.
According to the National Eating Disorder Association, orthorexia is an unhealthy obsession with eating “clean” or “healthful” foods. While caring about nutrition isn’t inherently problematic, orthorexia occurs when that focus becomes rigid and all-consuming, leading to extreme restriction, anxiety around food, and impairment in physical health or social functioning. It’s less about weight, and more about a compulsive pursuit of dietary purity at the expense of well-being.
What Intuitive Eating Actually Means
LC: Intuitive eating is very misunderstood, even by dietitians, and admittedly, by me. How do you explain it to someone encountering it for the first time?
NG: I explain it as bringing you back to the way you were when you entered the world. When you had no judgment about food being good or bad. When you weren’t making food choices based on what you think your body should look like.
Look at a toddler or an infant. They’re intuitive eaters. We’re all born intuitive eaters. They eat when they’re hungry and stop when they’re full. A breastfeeding baby stops when they’re full.
It’s about allowing all foods without guilt or shame and reconnecting to your body. We can’t forget all the messaging we’ve grown up with, but we can move closer to neutrality.
“If I Ate Intuitively, I’d Just Eat Oreos”
LC: A lot of people say, “If I ate intuitively, I’d eat Oreos after every meal.”
NG: That’s one of the most common things people say. I thought that too when I was struggling. I thought if I ate whatever I wanted, it would be French fries and pizza forever.
And honestly? In the beginning, that might happen. There’s often an uptick in previously restricted foods. It’s a response to dieting and restriction. There’s a recalibration period.
But it doesn’t last forever.
This is where body trust comes in. You need faith, especially when it feels hard. That’s why I recommend working with a dietitian trained in intuitive eating. Our bodies guide us toward health and balance.
Gentle Nutrition: Where Health Fits In
Intuitive eating isn’t anti-health. It’s anti-punishment.
NG: The tenth principle of intuitive eating is gentle nutrition. It’s the tenth for a reason. If you’re still early in the process and haven’t gotten out of dieting, health recommendations can feel like food rules.
Gentle nutrition honors both health and joy.
If someone has high LDL cholesterol, yes, I’m going to talk about viscous fiber. Lentils and beans. But the framing matters.
Instead of “You need to stop eating prosciutto,” it’s: “Let’s add lentil soup, especially if you already like it.”
It’s an additive approach before a subtractive one.
LC: Keep the white rice. Add the beans. That’s a win.
NG: Exactly. It’s honoring what the patient loves.
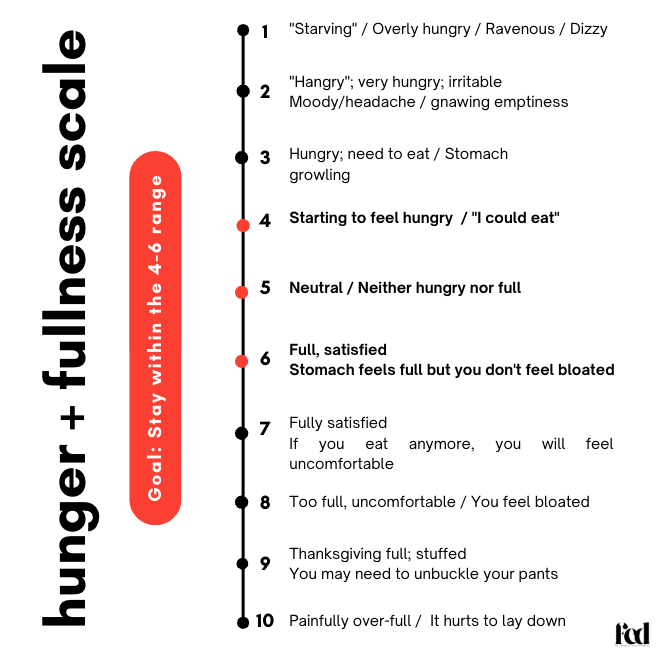
The Hunger Scale: Translating Body Cues
NG: Are you familiar with the hunger scale?
LC: Yes.
NG: I’ll think about it in numbers sometimes. I’ll notice I’m approaching an 8 — meaning I’m getting quite full and I’ll pause. Or I’ll think, I’m comfortably full right now.
For some clients, translating internal cues into a scale helps. It gives language to something that used to feel chaotic.
LC: I don’t do it by numbers. I visualize it as a spectrum. Am I closer to the top? The bottom? Or somewhere in the middle? Sometimes it’s as simple as asking: Am I good?
Even with something like a glass of wine. How am I feeling? What do I want? If I have more, how will I feel?
NG: Exactly. I’ll ask myself — if I have more, how will I feel? Do I want to feel that way? It’s less about rules and more about awareness.
Is Weight Ever a Useful Metric?
LC: Is body weight ever a useful clinical metric?
NG: I think about it like this…Do you know the show Love Is Blind? (a Netflix reality dating series where singles try to find a match and get engaged without ever seeing each other in person.) If I couldn’t see the person and didn’t know their weight, would my intervention change? Probably not.
We’d still focus on allowing all foods, putting weight loss on the back burner, and body acceptance.
Weight stigma is real. That affects lived experience. But the core intervention doesn’t change.
How Do You Measure Success?
LC: If weight is not a metric, how do you measure success?
NG: Interestingly, one way weight can be a metric is stability. Stability can signal a healthier relationship with food.
Other metrics are quality of life, less guilt and shame, connection to hunger and fullness cues.
I like to look at diet variety more than diet quality. Intuitive eaters tend to have more variety. When someone starts craving vegetables, that’s exciting.
GLP-1s and the Return of Thinness
LC: How are GLP-1s affecting weight stigma?
NG: Around 2020, body positivity and health at every size were really visible. Now, thin is in again in a big way.
Clients tell me it was easier to work on body neutrality a few years ago. Now, with GLP-1s, people feel like there’s an “easy fix.” They wonder if they should be taking it, and worry others are judging them for not taking it.
Society always has something to say.
We discussed the reality that weight tends to return after discontinuing GLP-1s, partly because energy needs decrease with weight loss, but appetite cues don’t always recalibrate. I wrote about this in a prior post.
NG: That’s a good moment for intuitive eating.
Private Practice: Who Seeks You Out?
NG: The people who seek me out feel guilt, shame, and obsessive thoughts around food. Often, there’s a history of dieting, whether an eating disorder, Weight Watchers, or chronic restriction. They don’t want to diet anymore, but they don’t know what to do next.
LC: What if that someone also wants weight loss?
NG: Almost everyone I work with wants to lose weight. We talk about it upfront. I don’t judge anyone.
But weight loss is not our primary intervention. Weight may go down, stay the same, or go up. We don’t know.
Building a Platform, Responsibly
Nicole’s Instagram presence, @thehungryclementine, grew organically from her recovery journey.
NG: I realized how much people appreciated hearing about my own experience. It made them feel less alone.
LC: But with a large platform comes responsibility. What kind of responsibility do you feel as a dietitian who is constantly posting about health and weight issues?
NG: We’re an evidence-based profession. I won’t share something theoretical without disclosing that. Accuracy matters.
Let’s See What We Have in Common
Sweet or savory breakfast?
NG: Sweet.
LC: Savory. Though I love a good pastry moment.
Plated meal person or grazer/snacker?
NG: Plated meal.
LC: Plated meal.
Cook at home or eat out?
NG: Cook at home. Mostly because I don’t want to spend the money eating out all the time.
LC: Cook at home. Because I genuinely love it. The shopping, the chopping, the having people over. All of it.
Meal planner or decide in the moment?
NG: Decide in the moment. Planning feels like work.
LC: Total planner. I like knowing what’s happening before it happens.
How often do you food shop?
NG: Maybe once a week at most. I keep frozen things on hand and pick up little things here and there.
LC: I’m probably there more often than I need to be. I enjoy the stroll.
Eat by the clock or eat by hunger?
NG: Hunger. I don’t really look at the time.
LC: Hunger. But my hunger seems aligned with the clock. If it’s 1:00 pm, I’m hungry.
Dessert most days or occasionally?
NG: Most days — though less than it used to be. I don’t need it every day anymore.
LC: Same.
Coffee or tea? Sweetened or unsweetened?
NG: Black coffee. Sometimes a latte. But a cozy black coffee? Love.
LC: Black coffee does not sound cozy to me. For me its coffee with frothy milk, no sugar.
Full-fat or low-fat dairy?
NG: Full fat. Though I don’t eat much dairy — mostly cheese, and that’s full fat.
LC: Full-fat milk. Non-fat plain yogurt. Full-fat cheese. A little of everything.
Sit-down meals or on-the-go eating?
NG: Predominantly sit-down.
LC: Sit-down.
Set the table or just put your plate down?
NG: Plate down.
LC: Placemat and napkin. Always. I can’t do a bare plate on a table.