Anti-Inflammatory Messaging
Can spices really lower inflammation, or are we just sipping on optimism?
It feels like everyone is walking around with a beverage lately. Regardless of the temperature, there always seems to be someone clutching an iced drink in some sort of earthy hue: turmeric lattes, matcha smoothies, ginger-lemon spritzes.
And people take them everywhere: on the subway, heading into workout classes, walking to work, leaving the gym. I’m never quite sure whether these are meal replacements or emotional support beverages.
From my vantage point, most people seem to be drinking them under the assumption that good things will follow. The term I hear tossed around most is anti-inflammatory.
But what does that actually mean? And are these powdered spices and wellness concoctions genuinely doing anything, or are we mostly just sipping optimism through a biodegradable straw?
What does anti-inflammatory even mean? Are the foods we eat making us swollen? I’m so confused.
Fair question. The word inflammation gets thrown around so much that it’s started to lose all meaning. Somewhere between green juice ads and wellness influencers blaming tomatoes for “toxins,” the concept went completely off the rails.
When scientists talk about inflammation, they’re usually not talking about feeling puffy after sushi night or your rings fitting tighter after a few margaritas. They’re referring to the immune system’s response to injury, stress, or perceived threat.
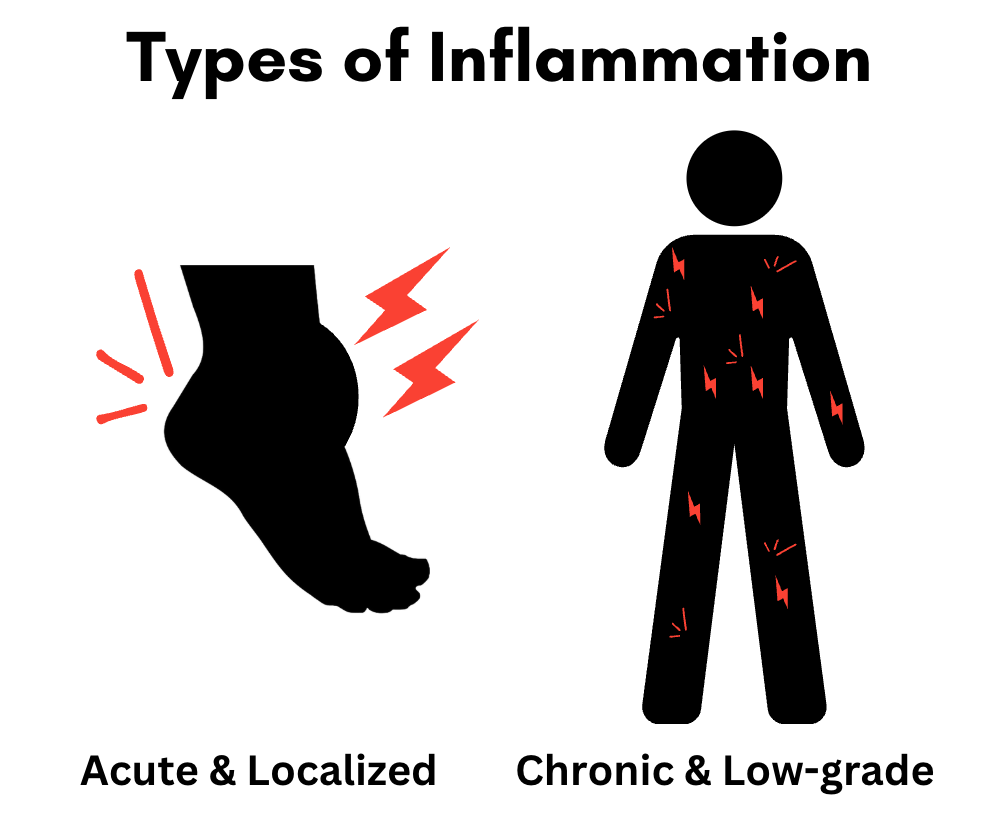
As I wrote in a prior post, some inflammation is normal and necessary. If you cut your finger, get sick, or twist your ankle, inflammation helps you heal. Blood flow increases, immune cells rush in, and the body gets to work repairing damage.
Chronic low-grade inflammation involves many of these same processes, just at a lower simmer and over a much longer period of time. Instead of a short-term, targeted response to injury, the immune system remains mildly activated throughout the body for months or even years. Over time, this has been linked to conditions like cardiovascular disease, type 2 diabetes, arthritis, and obesity.
So when someone says a food is anti-inflammatory, what they should be saying is that consuming this food has been associated with lower levels of certain inflammatory markers.
Not exactly marketing copy for a smoothie shop, but much more accurate.
How do I know if I have chronic inflammation?
Unlike a swollen ankle or a sore throat, chronic low-grade inflammation is harder to see or feel. Researchers and clinicians instead look for subtle changes in substances circulating in the blood, called biomarkers, that reflect inflammatory activity happening behind the scenes.
Noted. Let’s get back to the iced beverages. Is there evidence linking spices and anti-inflammation?
Surprisingly, yes.
Turmeric, ginger, and cinnamon have become the celebrity trio of the wellness world, showing up in everything from supplements to smoothies to beverages that sound vaguely medicinal. And unlike many nutrition trends, there’s actually some legitimate evidence behind the hype.
Turmeric, or more specifically curcumin, one of its main active compounds, has the strongest research. Multiple large reviews of clinical trials have found reductions in inflammatory markers like hsCRP.
Ginger also performs surprisingly well in studies, particularly for hsCRP.
Cinnamon has a smaller but still promising body of evidence, with some studies showing reductions in hsCRP and other inflammatory markers at doses of roughly 1.5–4 grams per day (about 1/4 -1 teaspoon).
Great! So I’m not just spinning my wheels with my $9 iced ginger turmeric matcha?
Sort of, but keep reading.
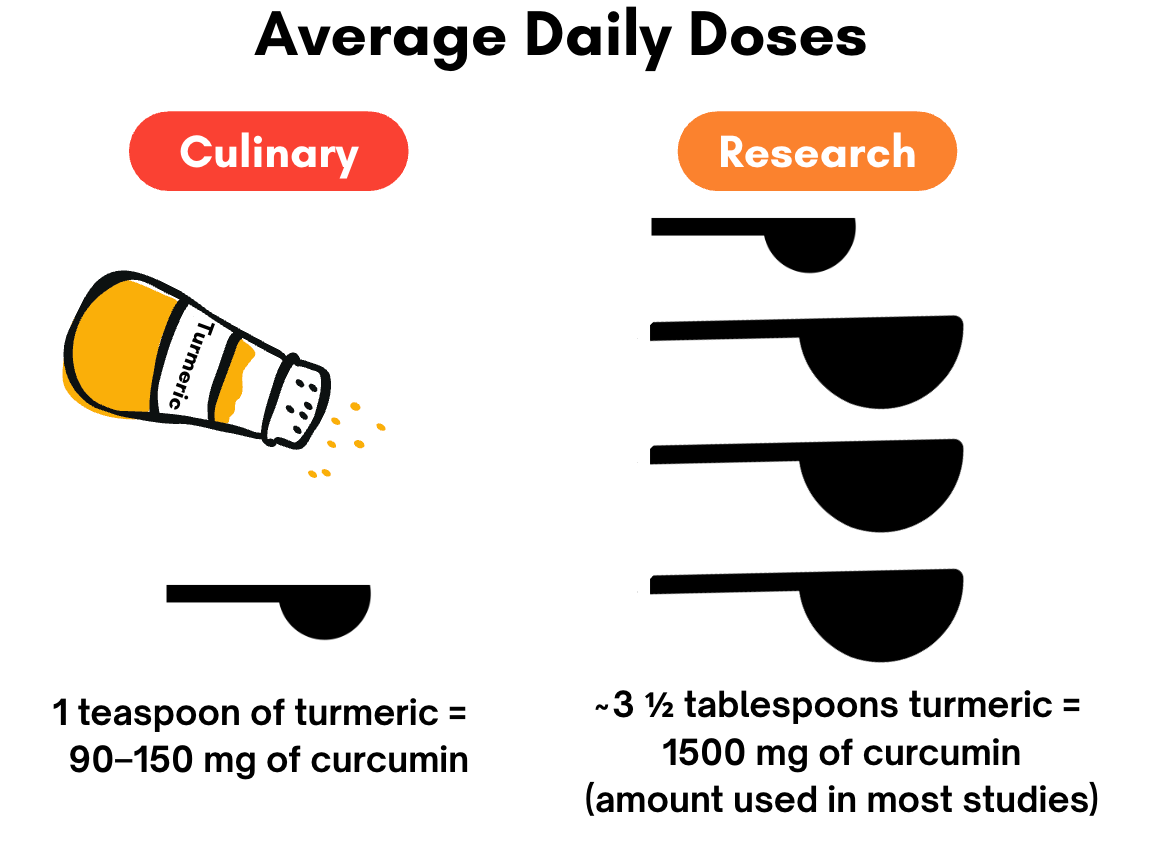
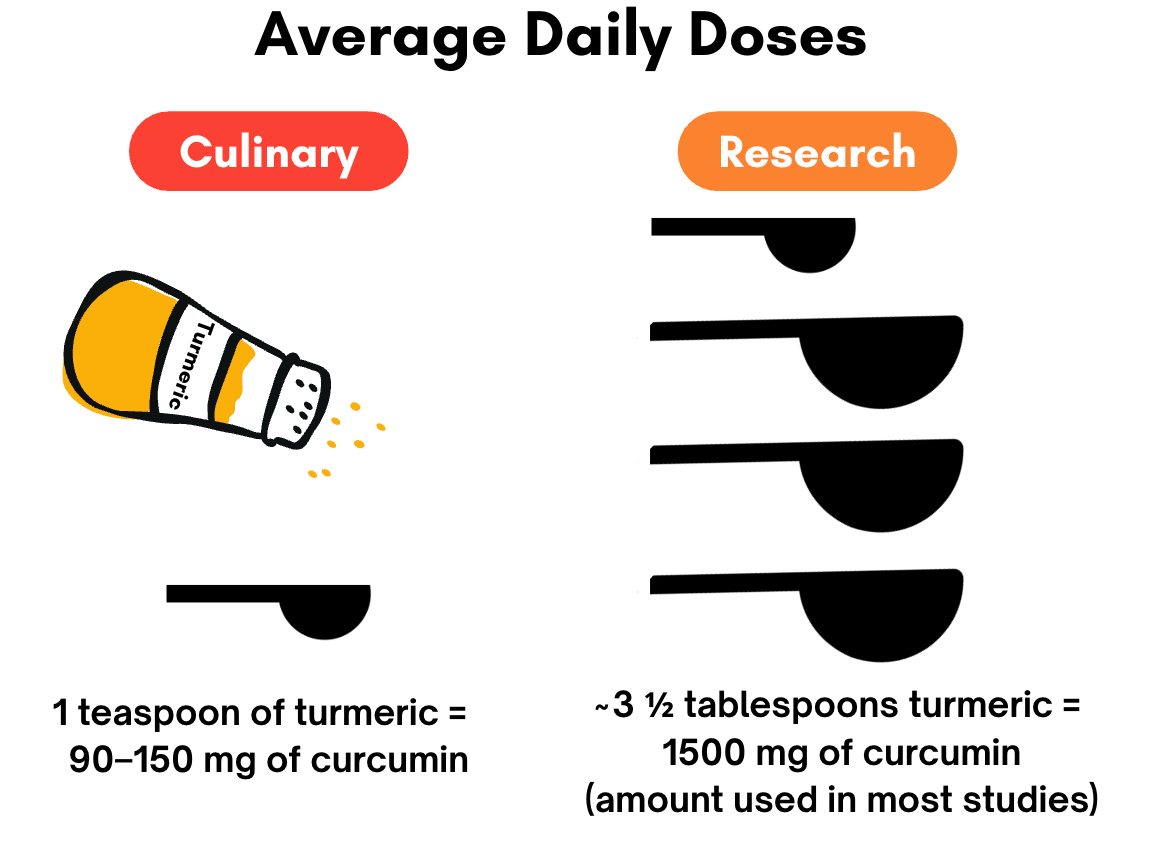
The evidence behind turmeric, ginger, and cinnamon is legitimate. But there’s an important nuance: most of the strongest effects were seen using concentrated supplements, not culinary amounts sprinkled into food.
In many studies, participants consumed hundreds, sometimes thousands, of milligrams of active compounds daily. That’s far more than what most people are getting from a latte, smoothie, or light dusting of turmeric on roasted vegetables.
Turmeric also has another complication: absorption.
Curcumin, turmeric’s main active compound, is notoriously difficult for the body to absorb on its own. Much of it passes through the digestive tract like a rumor in a group chat.
Black pepper, or more specifically piperine, despite its widespread use, does not appear to meaningfully improve curcumin bioavailability in controlled human studies and may carry potential drug interaction risks. The single most impactful strategy appears to be consuming curcumin with a fat-containing food or beverage, for example, whole milk or olive oil, which helps improve its solubility and absorption after digestion.
So no, adding a quarter teaspoon of turmeric to your scrambled eggs probably isn’t recreating a clinical trial. But that doesn’t mean culinary use is pointless. It just means we need to start thinking about spices as part of an overall dietary pattern.
So are spices actually doing something — or just making my food taste better?
Well, first: flavor matters. And spices making healthy food taste better is already a meaningful health contribution.
More importantly, emerging research suggests that whole foods and dietary patterns may matter more than isolated compounds anyway.
While the cinnamon, ginger, and turmeric trio are part of the blend, there are many others. And this gets at one of nutrition science’s biggest recurring themes: foods are more than the sum of their parts. Scientists call this the food matrix, the way fiber, fats, phytochemicals, and nutrients interact together inside real foods and meals.
So, your cinnamon oatmeal or turmeric lentils are probably not functioning like prescription anti-inflammatory drugs. But they may still contribute to a healthier overall dietary pattern, especially when they help make nutrient-dense foods more enjoyable, varied, and sustainable.
OK, I get the whole food matrix thing. But you did say most of the evidence for anti-inflammatory benefits comes from supplements. So how should I navigate supplementation?
First, always check with your doctor or pharmacist before starting a supplement. “Natural” does not automatically mean harmless.
Second, before spending money on supplements, it’s worth checking whether you actually have elevated inflammation to begin with. As mentioned, a blood test called hsCRP is currently one of the best clinical markers for chronic low-grade inflammation and can provide a more grounded starting point.
Among supplements, curcumin has some of the strongest evidence for helping lower hsCRP.
For supplementation, the best-studied approach is typically:
1,000 mg curcumin taken with a meal or beverage that has some fat
Taken consistently for 8–12 weeks
A few practical notes:
Turmeric tea may be comforting and culturally meaningful, but it’s unlikely to provide the curcumin levels used in clinical trials.
Supplement quality varies dramatically, so look for third-party testing such as USP, NSF, or ConsumerLab certification.
Turmeric, ginger, and cinnamon do appear to have anti-inflammatory effects in research settings, particularly turmeric/curcumin, which has the strongest evidence. But most studies used concentrated supplemental doses that are far higher than what people typically consume in cooking.
That doesn’t mean culinary use is meaningless.
Spices may still modestly support health as part of an overall dietary pattern, especially when they help make nutrient-dense foods more flavorful, varied, and sustainable.
In practice, this looks less like hacking inflammation with a single ingredient and more like consistently building meals around minimally processed foods, plants, fiber, healthy fats, and plenty of herbs and spices.
Think:
Cinnamon in oatmeal or yogurt
Ginger in stir-fries or marinades
Turmeric in soups, lentils, or rice dishes prepared with a little olive oil.
Nutrition is less about finding one magical compound and more about stacking small, realistic habits in your favor over time.